Health innovation and COVID-19 pandemic: Defining the need and response.
A question heard on the wards recently – how can we capture all the innovations that have emerged from the COVID-19 pandemic? I’m sure that there are similar questions in hospitals, GP surgeries and other organisations across the world.
In order to answer this question we need to start by defining innovation. The World Health Organization (which might want to drop the American spelling in light of recent political decisions) defines health innovation as follows:
“Health innovation is to develop new or improved health policies, systems, products and technologies, and services and delivery methods that improve people’s health, with a special focus on the needs of vulnerable populations.
- WHO engages in health innovation in the context of universal health coverage
- Health innovation adds value in the form of improved efficiency, effectiveness, quality, safety and/or affordability
- Health innovation can be in preventive, promotive, therapeutic, rehabilitative and/or assistive care”
In classic Public Health style WHO identifies 3 overlapping domains necessary to capture health innovation fully – science innovation (R&D), social innovation, and business innovation – each of which we can see in evidence in the wider pandemic response.
This is a useful definition for a number of reasons:
- it captures the breadth of activities encompassed by health innovation – this is not just about inventors producing gizmos (and is far removed from the majority of “innovations” mentioned in the context of the COVID-19 pandemic on social media)
- it reminds us that health innovation is not just about treatment – it’s also about prevention, rehabilitation and end of life decisions
- it relates to patients, families and staff
- it reminds us of those vulnerable populations most at risk – not just of infection but also social isolation, loss of income and poverty, and abuse
- it reminds us that an apparent advance is only useful if it improves outcomes – indeed the definition includes the words “improved” and “improve” in the first sentence, and “improved” in its subsequent bullet points
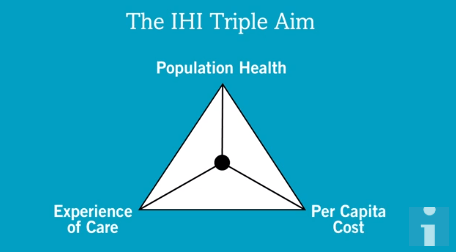
- it helps us link changes (potential innovations) with methodology for testing new ideas (quality improvement). The Institute for Healthcare Improvement’s Triple Aim provides a framework for optimising health system performance – improving population health, improving experience of care, reducing per capita cost – which has considerable overlaps with the WHO definition of health innovation. For anyone worrying about the words “reducing per capita cost”, the intention is to deliver more healthcare and improve outcomes within the funding available, rather than reducing healthcare budgets.
The definition also helps distinguish between essential Public Health measures and health innovation. If we look back to previous experience of novel coronavirus outbreaks e.g. SARS 2003, we see a similar range of effective Public Health interventions put in place – use of personal protective equipment (PPE), quarantine, testing, social distancing, legislation. Quarantine and social distancing have been central planks in responding to infectious disease outbreaks looking much further back to management of polio, smallpox (e.g. an outbreak in Sweden 1963) and the bubonic plague 1665-6.

Photograph: Gary Calton/The Observer
Indeed the word quarantine originates from earlier plague outbreaks, and derives from the Italian for forty days. These measures are necessary for an effective Public Health response during an infectious disease outbreak, and their omission can be disastrous as illustrated in numerous examples across the world during the COVID-19 pandemic.
The health innovations that emerge from the COVID-19 pandemic will depend on context, and will evolve during the different stages of the response. As the proverb goes, necessity is the mother of invention (Richard Franck, Northern Memoirs 1694).

Examples of innovation during the first wave of the COVID-19 pandemic include:
- Hospitals preparing for the influx of cases at the start of the pandemic, worried about the impact on the existing vulnerable and elderly inpatients, improving the way that hospitals and social care work together, helping support rapid but safe patient discharge.
- Hospitals dealing with massive pressures on beds and equipment during the peak of cases working heroically to adapt their pathways and delivery of care to support as many patients as possible, while minimising risk to patients and staff.
- Changes to IT systems in hospitals, including the electronic patient record. In one example a hospital had previously relied on paper forms for documentation of resuscitation status and decisions about anticipatory care planning (ACP) e.g. ward level care or escalation to intensive care. The forms differed between wards, and were stored in different folders between departments – e.g. at the end of bed, outside room, on a central trolley in the ward, or in medical notes in the doctors’ room. Accordingly, critical information can be hard to find during patient deterioration or cardiac arrest. Having the information easily available on an electronic system at ward and patient level could avoid delays in delivering care, or reduce the risk of providing unwanted interventions. However, changes to the electronic record typically take months or even years to approve and implement. With COVID-19 the system has been updated rapidly to display resuscitation status on the ward level display, and document ACP details in a tab in the individual patient’s electronic record.
- Information Governance rules typically state that information about patients cannot be routinely shared by email between organisations, or to patients/ family members. Death certification and registration processes have adapted to the COVID-19 pandemic. For example, in Scotland the interim arrangement for death registration during the pandemic allows remote death registration, with the death certificate emailed to the registry office and emailed to the family. This reduces the pressure and risk of infection for the family, hospital and registry office.
- Large numbers of recovering but still infectious COVID-19 patients, often with extensive rehabilitation needs, have required imaginative approaches from allied health professionals, and flexibility from hospital management in application and adaptation of PPE rules.
- Facilitating contact between patients and their families when hospital visiting is not allowed has been a challenge. Elderly and frail patients are often unfamiliar with technology, hospitals may have limited or no patient Wi-Fi, and equipment that has been handled or spoken into represents a potential route for spreading infection.
- Continuing to care for other patients – whether for emergencies or routine follow up – remains a challenge, and there are concerns that sick patients are staying away from hospital due to fear of catching COVID-19. GPs and hospital clinics are adapting, using telephone triage and telemedicine in novel ways, again requiring flexibility from Information Governance, and developing our understanding of what is acceptable to professionals, patients and families. These changes have occurred in a matter of weeks, sometimes achieving more over this short period than the same organisations have achieved in the preceding decade.

When we look back at this period at the end of the COVID-19 pandemic, we may have a number of responses to different innovations. Some measures will be viewed as specific to the pandemic, and discontinued. Others will have become integral to our work, and adopted without a second thought. Others still will be seen as transformative, and credited with making step changes in our response to the pandemic – e.g. in prevention (vaccination) or treatment. At a wider systems level however we will need to change our mindset towards innovation. We know from pandemic plans from across the world – both official and leaked reports – that some of the changes that occurred as crisis measures should have been in place before the pandemic. Similarly, some of the changes that have occurred in response to the pandemic seem so obvious that it is difficult to understand why they were not already in place. Alfred North Whitehead, writing over a century ago, and turning Franck’s ideas on their head, makes points that are useful in understanding this. He wrote that:
Inventive genius requires pleasurable mental activity as a condition for its vigorous exercise. ‘Necessity is the mother of invention’ is a silly proverb. ‘Necessity is the mother of futile dodges’ is much closer to the truth. The basis of growth of modern invention is science, and science is almost wholly the outgrowth of pleasurable intellectual curiosity. (Alfred North Whitehead)
Just as quality improvement work aims to avoid workarounds – those inefficient additional steps required to circumvent obstacles in a process – we should have ways to test and spread promising innovations without all the administrative and funding obstacles that delay progress during ordinary times. While it is difficult to feel light-hearted during a pandemic, cut off from family, friends and hobbies, and surrounded by news of mounting death tolls and missed opportunities to stem the pandemic, it is important to remember the joy of discovery and genuine progress. Individuals, organisations and society need to be able to embrace such advances, and remember that future crises and catastrophes can be prevented or at least ameliorated by the application of science, forward planning and cooperation across boundaries.
As we progress through this pandemic it will be fascinating to hear examples of health innovation. Please post your examples below or contact me via Twitter
Dr Graham Mackenzie, GPST2, Edinburgh, Scotland 26 April 2020.
This blog is also available as a PDF.

Reference:
Alfred North Whitehead, The Organisation of Thought, 1917, republished as The Aims of Education, 1929. Quote is from Chapter IV. Technical education and its relation to science and literature.
